Ashraf 2017 abdominal trauma
- 1. Blunt Abdominal Trauma By Ashraf M. Abdelkader Associate Professor General Surgery Banha University , EGYPT Consultant General Surgery KSH in Unizah , KSA
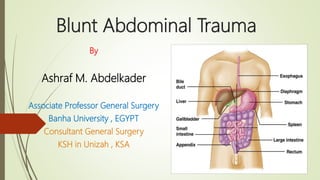
- 2. Background Anatomy Abdominal wall Anterior abdomen Flank Back 2
- 3. Abdominal cavity Intra-peritoneal Space Contents Retroperitoneal Space Contents Pelvic Cavity Contents
- 4. Introduction Abdominal trauma is regularly encountered in the emergency department. One of the leading cause of death and disability. Identification of serious intra-abdominal injuries is often challenging. Many injuries may not manifest during the initial assessment and treatment period
- 5. Epidemiology Peak incidence Abdominal Trauma 15 - 30yr Males > females Abdominal Injuries accounts for 10% of all deaths Estimates indicate that by 2020, 8.4 million people will die yearly. Abdominal trauma are major causes of morbidity and mortality. Combination injuries from bombs and explosive devices are on the increase
- 6. Types of Abdominal Trauma 1.Blunt Trauma 2.Penetrating Trauma -Stab -Gun shot Injury
- 8. MECHANISMS OF INJURY CRUSHING - Direct application of a blunt force to the abdomen SHEARING - Sudden decelerations apply a shearing force across organs with fixed attachments BURSTING - Raised intraluminal pressure by abdominal compression accurately in hollow organs can lead to rupture PENETRATION - Penetrating injury occurs directly from the object causing the injury or from kinetic energy released by the object. This can cause cavitation.
- 9. Blunt Trauma Abdomen RTA 75% of all blunt trauma abdominal injuries Direct blow 15% Fall down 5-6% Child Abuse Domestic Violence
- 10. - More common in elderly due to less resilience. - Blunt injuries causes solid organ trauma (spleen, liver and kidneys) more often than hollow viscera. - Multi organ injury and multiple system injury are also more common in blunt injury than in other types. Blunt Trauma Abdomen ( cont.)
- 11. PRESENTATION Varies widely from hemodynamic stability with minimal abdominal signs to complete cardiovascular collapse and may change from one to the other with alarming rapidity
- 12. Pattern of Injury in Blunt Abdominal Trauma Spleen 40.6% Colorectal 3.5% Liver 18.9% Diaphragm 3.1% Retroperitoneum 9.3% Pancreas 1.6% Small Bowel 7.2% Duodenum 1.4% Kidneys 6.3% Stomach 1.3% Bladder 5.7% Biliary Tract 1.1% * Rosen: Emergency Medicine (1998)
- 13. Prehospital Care The goal of pre-hospital is to deliver the pt to hospital for definitive care as rapidly as possible. ‘Scoop and Run’ Maintain airway & start I V line Care of spinal cord Communicate to medical control Rapid transport of patient to trauma centre
- 14. Initial Assessment and Resuscitation Primary survey Identification & treatment of life threatening conditions Airway , with cervical spine precautions Breathing and ventilation Circulation with hemorrhage control Disability +Neurologic Evaluation Exposure / Environmental Control
- 15. Emergency Care I V fluids Control external bleeding Dressing of wounds Protect eviscerated organs with a sterile dressing Stabilize an impaled object in place Give high flow oxygen Immobilize the patient with a fractured pelvis Keep the patient warm Analgesics
- 16. Secondary Survey AMPLE History A: Allergy(e.g. penicillin or aspirin) M: Medications(e.g. a beta-blocker or warfarin) P: Past medical history (e.g. previous surgery or anaesthetic mishap) L: Last meal(i.e. drink versus major meal) E: Event - What happened - To know injury mechanism (mode of injury) – to anticipate injury patterns and raise the index of suspicion for occult injury
- 17. MVC: What happened Speed Type of collision (frontal, lateral, sideswipe, rear, rollover) Vehicle intrusion into passenger compartment Types of restraints Deployment of air bag Patient's position in vehicle
- 18. PHYSICAL EXAMINATION General &Systemic Examination-to identify all occult injuries . Special attention to Back, Axilla , Perineum
- 19. Abdominal Examination Inspection : abdominal distension Distension Laceration Abrasion Seat Belt Sign
- 20. Examination Cullen’s Sign:1918 Bluish discoloration around umbilicus Diffusion of blood along periumbilical tissues or falciform ligament Hemoperitoneum Severe pancreatitis
- 21. Examination Grey-Turner’s Sign: (1877-1951) Bluish discoloration of the flanks Retroperitoneal Hematoma hemorrhagic pancreatitis. Kehr’s sign (1862-1916). Referred pain, Lt. shoulder irritation of the diaphragm (Splenic injury, free air, intra-abdominal bleeding)
- 22. Examination Labia and Scrotum : Pooling of blood from abdominal and pelvic cavities.
- 23. Examination Palpation: - Tenderness - Mass - Signs of peritonitis - # Ribs - Chest & Pelvic compression test Percussion : Dullness/ shifting dullness / hyper-resonance Auscultation : 1. +/- ve bowel sounds 2.. Bowel sounds in the thoracic cavity (Diaphragmatic rupture)
- 24. Rectal findings Check for gross blood - pelvic fracture Determine prostate position – high riding prostate – urethral injury Assess sphincter tone – neurologic status. NB. Foley’s catheter- monitor urine out put Nasogastric tube
- 25. INVESTIGATIONS Aim To identify To decide When (those with injury) (which ones (how quickly need laparotomy) this must be undertaken)
- 26. Investigations Laboratory tests FAST X-Ray Chest & Abdomen USG CT Scan Paracentasis Diagnostic Peritoneal Lavage Diagnostic Laparoscopy
- 27. Laboratory tests Complete haemogram with hematocrit, ABG Renal function tests Urine analysis – + ve of hematuria – genito urinary injury - ve of hematuria – does not rule out it Serum amylase / lipase or liver enzymes - se -suspicion of intraabdominal injuries
- 28. Focused Assessment with Sonography in Trauma (FAST) First used in 1996 Rapid , Accurate Sensitivity 86- 99% Can detect 100 mL of blood Cost effective Eliminates unnecessary CT scans Helps in management plan Four different views- Perihepatic Perisplenic Peripelvic space Pericardiac
- 29. FAST Algorithm FAST +Ve Unstable patient OT Stable patient CT -Ve Stable patient Observ. Unstable patient DPL +Ve OT -Ve The abdomen is not the Couse of shock
- 30. Plain X-Ray Chest & Abdomen Pneumothorax, Hemothorax Free air under diaphragm Nasogastric tube, bowel loops in the chest Elevation of the both /Single diaphragm Lower Ribs # -Liver /Spleen Injury Ground Glass Appearance – Massive Hemoperitoneum Obliteration of Psoas Shadow –Retroperitoneal Bleeding #vertebra
- 31. Paracentasis Four quadrant aspiration of abdomen. A Positive tap – blood , air , bile stained fluid. Negative tap doesn’t rule out injury. False negatives are as high as 22-60%
- 32. Diagnostic Peritoneal Lavage First described in 1965 Rapid & Accurate test used to identify intra-abdominal injuries Predictive value of greater than 90% Test is highly sensitive to presence of intraperitoneal blood However specificity is low Criteria for positive DPL: - Gross bloody tap - >1,00,000 RBCs per mm - > 500 white blood cells per mm - Elevated amylase level - Presence of bile or bacteria or faeces
- 33. Diagnostic Peritoneal Lavage Indications • Unexplained Shock • Altered sensorium (Head injury , Drug)
- 34. • Absolute : Peritonites Injured diaphragme Extraluminal air by x-ray Significant intraabdominal injury by CT scan Intraperitoneal perforation of the bladder by cystography CONTRAINDICATIONS • Relative : Previous abdominal operations (because of adhesions) Morbid obesity Gravid Uterus Advanced cirrhosis (because of portal hypertension and the risk of bleeding) Preexisting coagulopathy
- 35. What About DPL? Can be performed if –ve FAST in blunt abdominal trauma. If DPL +ve then emergency laparotomy. If DPL -ve then seek and treat other sources. Perform serial abdominal exams. Perform serial FAST exams. If patient stabilizes, then CT.
- 40. CT Scan Replacing DPL. Gold Standard Haemodynamically Stable Provides excellent imaging of pancreas, duodenum and Genitourinary system Standard for detection of solid organs injury. Determines the source and amount of bleeding Can reveal other associated injuries e.g. Vertebral & Pelvic # & injury in the thoracic cavity . High Specificity-95%
- 42. CT Scan Contraindication: Clear indication for Laparotomy Haemodynamically Unstable Allergy to contrast media
- 43. Diagnostic Modalities in Abdominal Trauma cont….. DPL US CT SCAN Sensitivity 100% 84% 89%** Specificity 97% 88% 98%** Accuracy 99% 86% 97% * Gruessner B, Mentges B, Duber C, et al : Sonography versus peritoneal lavage in blunt abdominal trauma. J Trauma 29:242, 1999. ** Meyer D M, Thal E R, Weigelt J A, et al: The role of abdominal CT in the evaluation of stab wounds to the back. J Trauma 29:1226, 1999.
- 44. DIAGNOSTIC LAPAROSCOPY Haemodynamically stable patients Inadequate/equivocal USG Mild hypotension or persistent tachycardia Persistent abdominal signs/symptoms It decreases non-therapeutic laparotomies Useful in penetrating injury Limitation :Retroperitoneal Injury
- 45. LAPAROSCOPY cont… Disadvantages: - Pneumoperitoneum may elevate ICP - General anesthesia usually necessary - Patient must be haemodynamically stable Complications: - Bleeding or injury - Gas embolism
- 47. Blunt abdominal trauma Haemodynamically Stable Shock due to other causes Haemodynamically Unstable LAPAROTOMY FAST DPL Follow up - ve + ve CT + ve - ve FAST
- 48. NON OPERATIVE MANAGEMENT OF BLUNT ABDOMINAL INJURY Patient haemodynamically stable after initial resuscitation: o Continuous patient monitoring for 48 hrs o Surgical team immediately available o Adequate ICU support and transfusion services available o admission for observation, serial hematocrit measurement, and repeat imaging
- 49. Laparotomy Indications Absolute criteria • Peritonitis (gross blood, bile or faeces) • Pneumoperitoneum or pneumoretroperitoneum • Evidence of diaphragmatic defect • Gross blood from stomach or rectum • Abdominal distension with hypotension • Positive diagnostic test for an injury requiring operative repair
- 50. Thank You
- 51. Solid Organ Injuries Grading of injured solid organs such as Spleen, Liver & Kidneys are on the basis of : 1- Subcapsular hematoma. 2- Capsular tear. 3- Parenchymal lacerations . 4- Avulsion of vascular pedicle.
- 52. Solid Organ Injuries Bleeds significantly and cause rapid blood loss Difficult to identify injury by physical exam Repeated assessment is required to make the diagnosis
- 53. SPLENIC INJURY Most common intra- abdominal organ to injured (40- 55%) 20% of splenic injuries due to left lower rib fractures Commonly arterial hemorrhage
- 54. SPLENIC INJURY Conservative management : (Success rate of conservative m/m is >80%) -Hemodynamic stability - Negative abdominal examination -Absence of contrast extravasation in CT - Absence of other indication of Laparotomy -Grade 1to 3 (Subcapsular Hematoma ,Laceration <3 cm) Monitoring o Serial abdo. Examinations & Haematocrit are essential
- 55. Splenic Injuries Operative Management: Capsular tears (I)- Compression & topical haemostatic agent Deep Laceration (II)- Horizontal mattress suture or Splenorrhaphy Major Laceration not involving hilum (IV)- Partial Splenectomy Hillar injury (V)–Total Splenectomy Grade IV-V: almost invariably require operative intervention Success rate of Splenic salvage procedure is 40-60%
- 56. Liver injury Liver is the largest organ in abdomen 2nd most common organ injured (35-45%) in BTA Driving and fighting responsible for 50% of deaths due to liver injury Usually venous bleeding 85% of all patients with blunt hepatic trauma are stable CT is the mainstay of diagnosis in stable pt.
- 57. Liver Injury Non Operative management : Haemodynamically Stable No other intra-abdominal injury require surgery < 2 units of BT required Hemoperitoneum <500 ml on CT Grade I-III(subcapsular & intr-perenchymal hematoma)
- 58. Liver Injury Operative management Packing - Bleeding can be stopped by packing of abdomen -Pack removed after 48 hr -hemostatic agents -34 % survival in packing only 50% liver injury have stop bleeding spontaneously by the time of surgery
- 59. Liver Injury Operative Management(Contd.) Suturing: -Simple suture -Deep mattress suture Laceration: -Mesh hepatorrhaphy -Omental flap to cover the laceration - Debridement Lobar Resection Liver Transplantation Ligate or repair damaged blood vessels & bile duct Mortality of liver injury is 10%
- 60. Pancreatic Injury Rare 10-20% of all abdominal injury Crush , Direct blow to abdo & Seat belt injury Associated with abdo. Duodenal injury, Vascular injury & liver injury Diagnosis – Difficult, High index of suspicion CECT Scan is helpful Serum amylase is a poor indicator Usually diagnose on Laparotomy Distal Pancreatic injury - Distal resection Pancreaticojejunostomy – Injury to Ampulla of Vater, Head & Body of Pancreas
- 61. Renal Injury Clinically not suspected & frequently overlooked Mechanism: Blunt , Penetrating # lower ribs or spinous process, Crush abdominal Pelvic injury Direct blow to flank or back Fall
- 62. Renal Injury Diagnosis 1.History ,Clinical examination 2. Presentation :Shock, hematuria & pain 3. Urine: gross or microscopic hematuria 4.X-ray KUB IVP 5. USG 6.CT Scan abdomen 7. Radionuclide Scan NB: The degree of hematuria may not predict the severity of renal injury
- 63. Renal Injury Classification of Injury Grade I : Contusion or Subcapsular Hematoma Grade II: Non Expanding Hematoma, <1 cm deep ,no extravasation Grade III: Laceration >1cm with urinary Extravasation Grade IV: Parenchymal Laceration deep to CM Junction Grade V: Renovascular injury
- 64. Management of Renal Injury Conservatively: 85% of blunt renal trauma Renal exploration : Indication Deep cortico-medullary Laceration with extravasation Large perinephric Hematoma Renovascular injury Uncontrolled bleeding Before Nephrectomy ,Contralateral Kidney should be assessed
- 65. Diaphragmatic Injury Incidence -0.8%-1.6% in BTA High index of suspicion required , may be missed. 40 to 50% are diagnosed immediately Presentation may be delayed Imaging Nasogastric tube seen in the thorax Abdominal contents in the thorax Elevated hemidiaphragm (>4 cm Lt vs Rt) Distortion of diaphragmatic margin. Lt- 69% , Rt -24% B/L- 15%
- 66. Hollow Viscus Injuries Gastric Injury : o Penetrating trauma MC o Blunt trauma abdomen 1% Duodenum o Isolated Duodenum injury rare Incidence - 3-5% Small Intestine& Colonic Injuries o Commonly Injured in Penetrating injury o Blunt Trauma -Incidence 5% -20%
- 67. Bladder Injury o Commonly in BTA o 70% of bladder Injury are associated with pelvic fracture . o Type 1.Extraperitoneal Rupture-by bony fragment 2. Intra-peritoneal Rupture- at dome
- 68. Vascular Injury Incidence 5-10% Highly lethal. Associated with extremely rapid rates of blood loss Exposure is difficult in Laparotomy Initial Control by digital pressure Heparinized saline (50U/ml) injected in both end of vessel Rx Lateral suture ,End to end Anastomosis & Interposition graft Mortality rate is very high
- 69. Injury Prevention 1.Primary: Prevent an injury from its occurrence in the first place: Educational activity such as anti-drink-driving campaigns , speed limit rule -Children should accompanied with parent 2.Secondary: Attempts to lesson the consequences of injury – making road & safer car, anti-locking brakes, air bags , helmets, seat belt 3. Tertiary: Minimize the effect of injury by health care by individuals & system.
- 70. Injury Prevention (Contd.) Speed is a critical factor ; a 10% increase speed translate into a 40% rise in the case fatality rate. Use of seat belt reduces the risk of death or serious injury by 45%. Air Bags reduces the risk of fatal injury by 30% & deaths by 11 %. Children Below 12yrs should be properly restraints in the back seat. Motorcycle experience death rate 35 time greater than car.
- 71. Summary Trauma is a massive & growing health burden worldwide ,which increasingly afflicts the young & productive age group. Repeated assessment is required to make the diagnosis Ultrasonography and peritoneal aspiration are rapid methods of determining or excluding the presence of Hemoperitoneum Conservative approach in Liver & Renal Injury Successful m/m of trauma requires integration of Pre- hospital ,in-hospital ,& rehabilitative care.
- 72. Thank You
Editor's Notes
- CT far more sensitive than FAST for detecting and characterizing abdominal injury in trauma. CT is the Gold Standard
