rheumatoid arthritis.pptx dr.ramjibanyadav
•Download as PPTX, PDF•
0 likes•1 view
ppt
Report
Share
Report
Share
Recommended
How I Think, How I Treat: Understanding Innovation in Multiple Myeloma—New Mo...

How I Think, How I Treat: Understanding Innovation in Multiple Myeloma—New Mo...PVI, PeerView Institute for Medical Education
Treatment of recurrent and resistant dermatomyositis and polymyositis in adults

Treatment of recurrent and resistant dermatomyositis and polymyositis in adultsMansoura university Hospital
Rheumatoid arthritis Part 1, case based approach with application of the late...

Rheumatoid arthritis Part 1, case based approach with application of the late...Internal medicine department, faculty of Medicine Beni-Suef University Egypt
More Related Content
Similar to rheumatoid arthritis.pptx dr.ramjibanyadav
How I Think, How I Treat: Understanding Innovation in Multiple Myeloma—New Mo...

How I Think, How I Treat: Understanding Innovation in Multiple Myeloma—New Mo...PVI, PeerView Institute for Medical Education
Treatment of recurrent and resistant dermatomyositis and polymyositis in adults

Treatment of recurrent and resistant dermatomyositis and polymyositis in adultsMansoura university Hospital
Rheumatoid arthritis Part 1, case based approach with application of the late...

Rheumatoid arthritis Part 1, case based approach with application of the late...Internal medicine department, faculty of Medicine Beni-Suef University Egypt
Similar to rheumatoid arthritis.pptx dr.ramjibanyadav (20)
How I Think, How I Treat: Understanding Innovation in Multiple Myeloma—New Mo...

How I Think, How I Treat: Understanding Innovation in Multiple Myeloma—New Mo...
Treatment of recurrent and resistant dermatomyositis and polymyositis in adults

Treatment of recurrent and resistant dermatomyositis and polymyositis in adults
Gliclazide 30 mg mr tablets smpc taj pharmaceuticals

Gliclazide 30 mg mr tablets smpc taj pharmaceuticals
Rheumatoid arthritis Part 1 Basics & guideline application on real life cases...

Rheumatoid arthritis Part 1 Basics & guideline application on real life cases...
Rheumatoid arthritis Part 1, case based approach with application of the late...

Rheumatoid arthritis Part 1, case based approach with application of the late...
RECENT ADVANCES IN TREATMENT OF RHEUMATOID ARTHRITIS

RECENT ADVANCES IN TREATMENT OF RHEUMATOID ARTHRITIS
IOSR Journal of Pharmacy (IOSRPHR), www.iosrphr.org, call for paper, research...

IOSR Journal of Pharmacy (IOSRPHR), www.iosrphr.org, call for paper, research...
Trihexyphenidyl 5mg tablets smpc taj pharmaceuticals

Trihexyphenidyl 5mg tablets smpc taj pharmaceuticals
C19 nice dapagliflozin in combination therapy for treating type2 diabetes 2013

C19 nice dapagliflozin in combination therapy for treating type2 diabetes 2013
More from RAMJIBANYADAV2
More from RAMJIBANYADAV2 (19)
DENGUE FEVER BY DR.RADHE.pptx CIVIL HOSPITAL NEPAL

DENGUE FEVER BY DR.RADHE.pptx CIVIL HOSPITAL NEPAL
Hypocalcemia-PPT dr.ram jiban yadav nepal civil service hospital

Hypocalcemia-PPT dr.ram jiban yadav nepal civil service hospital
Recently uploaded
Escort Service Call Girls In Sarita Vihar,, 99530°56974 Delhi NCR

Escort Service Call Girls In Sarita Vihar,, 99530°56974 Delhi NCR9953056974 Low Rate Call Girls In Saket, Delhi NCR
Russian Call Girls in Delhi Tanvi ➡️ 9711199012 💋📞 Independent Escort Service...

Russian Call Girls in Delhi Tanvi ➡️ 9711199012 💋📞 Independent Escort Service...Call Girls In Delhi Whatsup 9873940964 Enjoy Unlimited Pleasure
Recently uploaded (20)
Call Girl Number in Vashi Mumbai📲 9833363713 💞 Full Night Enjoy

Call Girl Number in Vashi Mumbai📲 9833363713 💞 Full Night Enjoy
💎VVIP Kolkata Call Girls Parganas🩱7001035870🩱Independent Girl ( Ac Rooms Avai...

💎VVIP Kolkata Call Girls Parganas🩱7001035870🩱Independent Girl ( Ac Rooms Avai...
Best Rate (Hyderabad) Call Girls Jahanuma ⟟ 8250192130 ⟟ High Class Call Girl...

Best Rate (Hyderabad) Call Girls Jahanuma ⟟ 8250192130 ⟟ High Class Call Girl...
Russian Escorts Girls Nehru Place ZINATHI 🔝9711199012 ☪ 24/7 Call Girls Delhi

Russian Escorts Girls Nehru Place ZINATHI 🔝9711199012 ☪ 24/7 Call Girls Delhi
VIP Call Girls Pune Sanjana 9907093804 Short 1500 Night 6000 Best call girls ...

VIP Call Girls Pune Sanjana 9907093804 Short 1500 Night 6000 Best call girls ...
(👑VVIP ISHAAN ) Russian Call Girls Service Navi Mumbai🖕9920874524🖕Independent...

(👑VVIP ISHAAN ) Russian Call Girls Service Navi Mumbai🖕9920874524🖕Independent...
Bangalore Call Girls Hebbal Kempapura Number 7001035870 Meetin With Bangalor...

Bangalore Call Girls Hebbal Kempapura Number 7001035870 Meetin With Bangalor...
Call Girls Service Pune Vaishnavi 9907093804 Short 1500 Night 6000 Best call ...

Call Girls Service Pune Vaishnavi 9907093804 Short 1500 Night 6000 Best call ...
Escort Service Call Girls In Sarita Vihar,, 99530°56974 Delhi NCR

Escort Service Call Girls In Sarita Vihar,, 99530°56974 Delhi NCR
Call Girls Service Bellary Road Just Call 7001305949 Enjoy College Girls Service

Call Girls Service Bellary Road Just Call 7001305949 Enjoy College Girls Service
CALL ON ➥9907093804 🔝 Call Girls Hadapsar ( Pune) Girls Service

CALL ON ➥9907093804 🔝 Call Girls Hadapsar ( Pune) Girls Service
VIP Call Girls Pune Vrinda 9907093804 Short 1500 Night 6000 Best call girls S...

VIP Call Girls Pune Vrinda 9907093804 Short 1500 Night 6000 Best call girls S...
Artifacts in Nuclear Medicine with Identifying and resolving artifacts.

Artifacts in Nuclear Medicine with Identifying and resolving artifacts.
Russian Call Girls in Pune Riya 9907093804 Short 1500 Night 6000 Best call gi...

Russian Call Girls in Pune Riya 9907093804 Short 1500 Night 6000 Best call gi...
Call Girls Yelahanka Bangalore 📲 9907093804 💞 Full Night Enjoy

Call Girls Yelahanka Bangalore 📲 9907093804 💞 Full Night Enjoy
Russian Call Girls in Delhi Tanvi ➡️ 9711199012 💋📞 Independent Escort Service...

Russian Call Girls in Delhi Tanvi ➡️ 9711199012 💋📞 Independent Escort Service...
Call Girls In Andheri East Call 9920874524 Book Hot And Sexy Girls

Call Girls In Andheri East Call 9920874524 Book Hot And Sexy Girls
Kesar Bagh Call Girl Price 9548273370 , Lucknow Call Girls Service

Kesar Bagh Call Girl Price 9548273370 , Lucknow Call Girls Service
Call Girls Service Jaipur Grishma WhatsApp ❤8445551418 VIP Call Girls Jaipur

Call Girls Service Jaipur Grishma WhatsApp ❤8445551418 VIP Call Girls Jaipur
rheumatoid arthritis.pptx dr.ramjibanyadav
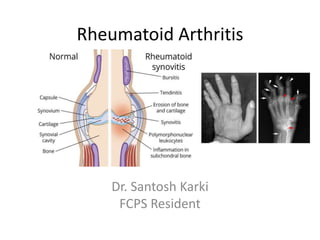
- 1. Rheumatoid Arthritis Dr. Santosh Karki FCPS Resident
- 36. • General principles and overview of management of rheumatoid arthritis in adults
- 39. 1. Therapy with DMARDs should be started as soon as the diagnosis of RA is made. 2. Treatment should be aimed at reaching a target of sustained remission OR, low disease activity in every patient. 3. Monitoring should be frequent in active disease (every 1–3 months); if there is no improvement by at most 3 months after the start of treatm or the target has not been reached by 6 months, therapy should be adju RA treatment that initiation of DMARD therapy should be immediate, since the disease will not remit spontaneously. This is a central theme in the care of patients with RA and aka Treat-to-Target approach.
- 40. 4. MTX should be part of the first treatment strategy. 5. In patients with a contraindication to MTX (or early intolerance), Leflunomide or Sulfasalazine should be considered as part of the (first) treatment strategy. MTX remains the anchor drug in RA it an efficacious csDMARD by itself and also with combination therapies, either with GC or with other csDMARDs, bDMARDs or tsDMARDs.
- 41. 6. Short-term GCs should be considered when initiating or changing csDMAR in different dose regimens and routes of administration, but should be tapered and discontinued as rapidly as clinically feasible. GCs is used as bridging therapy until csDMARDs exhibit their efficacy and that tapering GC rapidly is important. Failure to sustain the treatment target on tapering or withdrawal of GC after the bridging phase should be regarded as failure of this therapeutic phase and thus elicit the institution of a bDMARD or a tsDMARD added to the csDMARD.
- 43. 7. If the treatment target is not achieved with the first csDMARD strategy, in the absence of poor prognostic factors, other csDMARDs should be cons 8. If the treatment target is not achieved with the first csDMARD strategy, when poor prognostic factors are present, a bDMARD should be added; JAK-inhibitors may be also considered. Poor prognostic factors
- 45. 9. bDMARDs and tsDMARDs* should be combined with a csDMARD; in patients who cannot use csDMARDs as comedication, IL-6 pathway inhibitors and tsDMARDs* may have some advantages compared with other bDMARDs. 10. If a bDMARD or tsDMARD* has failed, treatment with another bDMARD or a tsDMARD* should be considered; if one TNF- or IL-6 receptor inhibitor therapy has failed, patients may receive an agent with another mode of action or a second TNF- or IL-6 receptor inhibitor 11. After GCs have been discontinued and a patient is in sustained remission, dose reduction of DMARDs (bDMARDs/tsDMARDs and/or csDMARDs) may be considered.