Niosomes (Formulation and evaluation).pptx
- 1. NIOSOMES: FORMULATION AND EVALUATION SUBMITTED BY: PRACHI PANDEY, RAHUL PAL M. PHARM (PHARMACEUTICS), IIIRD SEM. DEPARTMENT OF PHARMACEUTICS, NIMS INSTITUTE OF PHARMACY, NIMS UNIVERSITY, JAIPUR, RAJASTHAN, 303121, INDIA.
- 2. INTRODUCTION Niosomes are a novel drug delivery system that encapsulates the medication in a vesicular system made up of non ionic surfactants. In 1909, Paul Ehrlich named niosomes as “magic bullet” as he proposed the strategies of targeted drug delivery system without damaging the surrounding cells. The vesicle is made up of a bilayer of non-ionic surfactants, thus the name niosomes. Niosomes are extremely small and microscopic (on a nanometric scale). Despite having a similar structure to liposomes, they have several advantages over them. Niosomes are biocompatible, non-immunogenic, and biodegradable in nature and exhibit flexibility in their structured characterization Niosomes
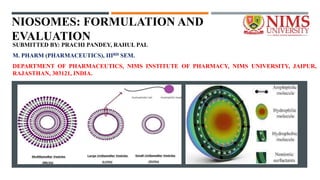
- 3. INTRODUCTION The main purpose of developing vesicular structures are modification of distribution profiles and targeted delivery of the drug Based on the vesicle size, niosomes can be divided into three groups. I. Small unilamellar vesicles (SUV, size=0.025-0.05 μm), II. Multilamellar vesicles (MLV, size=>0.05 μm), and III. Large unilamellar vesicles (LUV, size=>0.10 μm). Niosomes
- 4. LIPOSOMES V/S NIOSOMES Feature Niosomes Liposomes Composition Uncharged single-chain surfactants and cholesterol Double-chain phospholipids (neutral or charged) and cholesterol Cost Cheaper More expensive Preparation Easier, less specific process Complex, requires specific phospholipids Stability Highly stable Can be less stable Permeability Higher permeability for ions and small molecules Lower permeability Drug entrapment efficiency Can be higher Can be lower Targeted delivery Potential for targeting with specific surfactants Potential for targeting with specific phospholipids Commercial availability Limited More widely available Examples of use Topical drug delivery, gene delivery, cosmetic applications Drug delivery, cosmetics, vaccines
- 5. COMPOSITIONS OF NIOSOMES Component Function Non-ionic Surfactant Forms the bilayer membrane, affecting permeability and drug entrapment. Cholesterol Stabilizes the membrane, influencing fluidity and targeting ability. Hydrating Medium Provides the internal environment for encapsulated drugs. Charge Molecule Improves stability, targeting, and sometimes drug release.
- 6. COMPOSITIONS OF NIOSOMES Component Examples Required Non-ionic surfactant Span 60, Span 20, Tween 80, Tween 20, Pluronic F127, Cremophor EL, Solutol HS15 Yes Cholesterol Yes, Optional, Optional, Optional, Optional, Optional, Optional As per the need Hydrating medium Water, Buffered solution (e.g., PBS), Alcohol/water mixture, Organic solvents (e.g., ethanol, methanol), Ionic solutions Yes Charge molecule None (neutral niosomes), Dicetylphosphate (anionic), Stearylamine (cationic), Phosphatidylglycerol (anionic), Chitosan (cationic) Optional
- 8. NIOSOMES ENCAPSULATION In the formulation of niosomes, the selection of surfactants is based on hydrophilic-lipophilic balance (HLB) value. HLB values between 4 and 8 recommended for the facile formation of niosomes and surfactants with an HLB value of more than 8 are required to optimize cholesterol concentration. However, it has been widely observed that HLB value between 4 and 8 is highly recommended for better encapsulation efficiency, of niosomes. For example, long stearyl and short lauryl chain length increase and decrease the entrapment efficiency of niosomes, respectively. Long hydrophilic chains result in increased encapsulation of hydrophilic drugs, and long hydrophobic chains result in improved encapsulation of lipophilic drugs.
- 9. NON IONIC SURFACTANTS Long Hydrophilic Chains and Increased Encapsulation of Hydrophilic Drugs: Surfactants with longer hydrophilic chains create larger aqueous compartments within the niosome bilayer. This provides more space for water-soluble drugs to reside, leading to higher encapsulation efficiency. Example: Span 60 (HLB 4.7) has a longer hydrophilic chain compared to Span 20 (HLB 8.6). Studies have shown that using Span 60 in niosomes resulted in significantly higher encapsulation efficiency of the hydrophilic drug gentamicin, compared to formulations using Span 20.
- 10. NON IONIC SURFACTANTS Long Hydrophobic Chains and Improved Encapsulation of Lipophilic Drugs: Long hydrophobic chains increase the affinity of the niosome bilayer for lipid-soluble drugs. These drugs can partition and entrap themselves within the bilayer structure, leading to improved encapsulation. Example: Tween 80 (HLB 15) has a longer hydrophobic chain compared to Tween 20 (HLB 16.7). Niosomes prepared with Tween 80 demonstrated superior encapsulation of the lipophilic drug curcumin compared to those made with Tween 20.
- 11. CHARGE INDUCERS In niosomes, which are microscopic spheres used for drug delivery, charge inducers offer several benefits. They primarily improve the stability of the niosomes by introducing a positive or negative charge on their surface. This charge creates a repulsive force between individual niosomes, preventing them from clumping together and compromising the formulation. Additionally, a higher zeta potential (a measure of the charge) indicates greater stability. This enhanced stability ensures efficient transport and delivery of the encapsulated drug to its target site.
- 12. CHARGE INDUCERS Negative charge inducers Enhances stability by preventing aggregation; May be useful for targeting niosomes to positively charged cells; Can help to reduce interaction with serum proteins Example: Dicetyl phosphate, dihexadecyl phosphate, and lipoamino acid Positive charge inducers Enhances stability by preventing aggregation; Can be used to target niosomes to negatively charged cells; May promote drug release in acidic environments Example: Stearylamine and cetylpridinium chloride, help to stabilize the vesicles.
- 13. HYDRATION MEDIUM The hydration medium used during the formation of niosomes plays a crucial role in determining their characteristics and performance. Depending on the choice of hydration medium, niosomes can exhibit varied drug encapsulation efficiency, particle size, and stability. For instance, the use of phosphate buffer saline (PBS) as a hydration medium can result in the formation of small-sized niosomes with high encapsulation efficiency, making them suitable for the delivery of hydrophilic drugs such as doxorubicin or 5-fluorouracil, which require high entrapment efficiencies for effective therapeutic outcomes. On the other hand, employing ethanol as a hydration medium can lead to the formation of larger niosomes with improved stability and prolonged drug release profiles, making them ideal for the delivery of lipophilic drugs like paclitaxel or curcumin, where sustained release is desired to maintain therapeutic concentrations over an extended period.
- 14. HYDRATION MEDIUM The hydration medium used during the formation of niosomes plays a crucial role in determining their characteristics and performance. Depending on the choice of hydration medium, niosomes can exhibit varied drug encapsulation efficiency, particle size, and stability. For instance, the use of phosphate buffer saline (PBS) as a hydration medium can result in the formation of small-sized niosomes with high encapsulation efficiency, making them suitable for the delivery of hydrophilic drugs such as doxorubicin or 5-fluorouracil, which require high entrapment efficiencies for effective therapeutic outcomes. On the other hand, employing ethanol as a hydration medium can lead to the formation of larger niosomes with improved stability and prolonged drug release profiles, making them ideal for the delivery of lipophilic drugs like paclitaxel or curcumin, where sustained release is desired to maintain therapeutic concentrations over an extended period.
- 16. PEGYLATION Pegylation is a process where polyethylene glycol (PEG), a biocompatible and hydrophilic polymer, is attached to the surface of niosomes. This modification offers several advantages for drug delivery: Benefits of Pegylation: Increased Stability: PEG creates a steric barrier, preventing proteins and other molecules in the blood from adhering to the niosome surface. This reduces aggregation and opsonization (recognition by immune cells), leading to a longer circulation time in the bloodstream. Improved Bioavailability: Enhanced stability means more niosomes reach the target site, delivering their cargo. Reduced Toxicity: PEG is generally non-toxic and non-immunogenic, minimizing potential side effects. Enhanced Targeting: Specific ligands (molecules that bind to receptors) can be attached to PEG, enabling niosomes to target specific cells or tissues. Methods of Pegylation: Pre-conjugated Surfactants: Surfactants with pre-attached PEG chains can be incorporated into the niosome bilayer. Post-insertion Methods: PEG molecules can be chemically linked to the existing niosomal surface after preparation.
- 17. OPSONISATION Opsonization is a crucial process in the body's immune system where molecules called opsonins coat foreign particles, like niosomes, making them more recognizable and palatable for phagocytes like macrophages. These phagocytes then engulf and eliminate the foreign particles. In the context of niosomes, opsonization can have both positive and negative impacts: Positive Impacts: Enhanced Clearance: Opsonization can actually be beneficial for niosomes designed for short-term drug delivery. It facilitates rapid uptake by phagocytes, leading to efficient drug release at the target site. This can be useful for drugs requiring prompt action or localization within specific tissues. Stimulating Immune Response: In some cases, niosomes can be intentionally designed to induce a controlled immune response, particularly for vaccines or immunotherapies. Opsonization helps antigen-presenting cells recognize and process the encapsulated antigens, ultimately leading to a stronger immune response. Negative Impacts: Reduced Circulation Time: For niosomes meant for sustained or targeted drug delivery, opsonization can be detrimental. Rapid clearance by phagocytes reduces their circulation time, hindering their ability to reach the target site and release the drug effectively. This can limit the overall therapeutic efficacy. Potential Immune Reactions: In some individuals, excessive opsonization can trigger unwanted immune reactions, particularly for niosomes carrying large or immunogenic payloads. This can lead to inflammation, allergic reactions, or even organ damage.
- 18. STEALTH Stealth, also known as long-circulating properties, is a crucial aspect of niosome design for efficient drug delivery. It refers to the ability of niosomes to evade the body's natural defense mechanisms, namely the mononuclear phagocyte system (MPS), for an extended period in the bloodstream. This allows them to circulate longer, accumulate at the target site more effectively, and ultimately deliver the encapsulated drug with greater potency. Niosomes achieve stealth properties: Steric Repulsion: The primary strategy involves attaching polyethylene glycol (PEG) molecules to the niosome surface. PEG forms a hydrophilic "cloud" around the niosome, creating a steric barrier. This barrier repels proteins in the blood plasma that would otherwise opsonize (mark) the niosome for uptake by macrophages, the key players in the MPS. Reduced Protein Adsorption: PEGylation also minimizes the direct interaction between niosomes and plasma proteins. This further reduces opsonization and subsequent clearance by the MPS. Tailored Charge: Modifying the surface charge of niosomes can also contribute to stealth. A slightly negative charge, for example, can repel negatively charged cell membranes of macrophages, making them less likely to engulf the niosome.
- 19. NIOSOMAL FORMULATION Niosomal formulation can be followed by these following process 1. Thin-film hydration method, 2. Ether injection method, 3. Reverse-phase evaporation method, 4. Transmembrane pH gradient drug uptake process, 5. Bubble method, and 6. Micro-fluidization method
- 20. THIN FILM HYDRATION METHOD a. Dissolve drug, non-ionic surfactant(s), and cholesterol in a volatile organic solvent (e.g., chloroform, methanol). b. Remove the solvent using a rotary evaporator, forming a thin film on the flask wall. c. Hydrate the film with an aqueous phase (buffer, saline) under gentle agitation. d. Optionally, apply sonication or homogenization to improve dispersion. e. Separate unentrapped drug by centrifugation or ultrafiltration. f. Size and entrapment efficiency can be optimized by varying ingredients and processing parameters. Advantages: Simple, versatile, suitable for various drugs. Disadvantages: May have low encapsulation efficiency, possibility of residual solvent. THIN FILM HYDRATION METHOD
- 21. ETHER INJECTION METHOD a. Dissolve drug in a water-miscible organic solvent (e.g., diethyl ether). b. Inject the organic phase containing drug into a heated aqueous phase containing surfactant and cholesterol. c. Rapid diffusion and solvent evaporation induce niosome formation. d. Remove residual solvent by dialysis or ultrafiltration. Advantages: High encapsulation efficiency, rapid process. Disadvantages: Limited solvent choice, potential drug instability due to high temperatures. ETHER INJECTION METHOD
- 22. REVERSE PHASE EVAPORATION METHOD a. Dissolve drug, surfactant(s), and cholesterol in an organic phase. b. Add an aqueous phase containing a helper lipid (e.g., dicetylphosphate). c. Evaporate the organic phase under reduced pressure. d. Niosomes form spontaneously due to micelle-to-vesicle transition. e. Remove helper lipid by ultrafiltration if needed. Advantages: High encapsulation efficiency, good control over size and stability. Disadvantages: Requires helper lipid, potential for drug-lipid interactions. REVERSE PHASE EVAPORATION METHOD
- 23. TRANSMEMBRANE PH GRADIENT DRUG UPTAKE PROCESS a. Load niosomes with a pH-sensitive drug in an acidic environment. b. Raise the external pH using a buffered solution. c. The drug ionizes and becomes trapped within the niosomal core. d. Remove free drug by ultrafiltration. Advantages: Targeted drug delivery, high encapsulation efficiency for ionizable drugs. Disadvantages: Complex process, limited to ionizable drugs. Transmembrane pH Gradient Drug Uptake Process
- 24. BUBBLE METHOD Dissolve drug, surfactant(s), and cholesterol in an organic phase. Sparge the solution with gas (e.g., nitrogen) to form microbubbles. Add an aqueous phase and continue sparging. Solvent evaporation and shear stress from bubbles induce niosome formation. Separate niosomes by centrifugation or ultrafiltration. Advantages: Continuous process, high scalability, potential for large-scale production. Disadvantages: Complex setup, control over size and encapsulation efficiency might be challenging. BUBBLE METHOD
- 25. MICRO FLUIDIZED METHOD a. Mix drug, surfactant(s), and cholesterol in an aqueous phase. b. Subject the mixture to high pressure and shear stress in a microfluidic device. c. The intense forces disrupt and reform vesicles, generating niosomes. d. Optimize pressure and flow rate for desired size and distribution. Advantages: Narrow size distribution, high entrapment efficiency, continuous process. Disadvantages: Requires specialized equipment, high initial investment. MICRO FLUIDIZED METHOD
- 26. EVALUATION IN-VITRO Particle size and size distribution: DLS, NTA Zeta potential: Zetameter Polydispersity index (PDI): Calculated from size distribution data Morphology: TEM, SEM Entrapment efficiency: Separation of free and encapsulated drug In vitro release: Simulated dissolution studies in relevant media Stability studies: Monitoring changes in size, zeta potential, etc., over time Cytotoxicity studies: Evaluation of potential toxicity on cell lines. IN-VIVO Biodistribution studies: Tracking niosomal distribution in organs and tissues Pharmacokinetic studies: Monitoring drug concentration in blood and plasma over time Target site accumulation: Assessing targeting efficiency to specific tissues or cells Therapeutic efficacy studies: Evaluating the drug's therapeutic effect in animal models Toxicity studies: Assessing potential side effects in animals.
- 27. EVALUATION (IN VITRO) Parameter Description Accepted Limit Instrument Formula Particle size Average diameter of niosomes < 500 nm (optimal) Dynamic Light Scattering (DLS) D = K1 * λ / θ Where: D = diameter, K1 = proportionality constant, λ = wavelength of light, θ = scattering angle Zeta potential Surface charge of niosomes ± 30 mV (absolute value) Zeta potential analyzer ζ = (μ ε / η) * V Where:ζ = zeta potential, μ = electrophoretic mobility, ε = dielectric constant of medium, η = viscosity of medium, V = electric field strength Polydispersity index (PDI) Size distribution of niosomes 0.1 - 0.3 (narrow distribution) DLS PDI = σ² / D² Where: σ² = variance of particle size distribution Morphology Shape and surface characteristics of niosomes Spherical, smooth surface Transmission Electron Microscopy (TEM) or Scanning Electron Microscopy (SEM) Image analysis software to measure size, shape, and surface features Entrapment efficacy Percentage of drug encapsulated within niosomes > 50% (desired) Spectrophotometry, HPLC, other drug- specific methods % Entrapment = (Encapsulated drug / Total drug) * 100
- 28. EVALUATION (IN VIVO) Drug Category Desired Goal Animal Model Techniques Employed Outcome Measures Antibiotics Improved efficacy, reduced side effects, targeted delivery Mice, rats Tail vein injection, subcutaneous injection, oral gavage Bacterial burden reduction, survival rates, blood drug levels, tissue distribution, histopathology Anticancer drugs Enhanced bioavailability, improved tumor targeting, reduced systemic exposure Mice, rats Intravenous injection, intratumoral injection Tumor growth inhibition, survival rates, blood drug levels, tumor drug accumulation, biodistribution studies Vaccines Increased immunogenicity and protection Mice, rabbits Intramuscular injection, subcutaneous injection Antibody response, protection against pathogen challenge, immune cell activation Gene therapy Efficient gene delivery to target tissues Mice, rats Intravenous injection, local injection Transgene expression levels, functional analysis of expressed protein, biodistribution studies
- 29. APPLICATION OF NIOSOMES Drug Delivery: Niosomes can encapsulate various drugs, enhancing their bioavailability, stability, and targeted delivery. They show potential in treating: Skin disorders: Topical niosomal formulations for antifungal (e.g., clotrimazole), anti-inflammatory (e.g., diclofenac), and anti-acne (e.g., isotretinoin) drugs are being explored and marketed (e.g., Vesigel®, Diflucan®). Ophthalmic diseases: Niosomal formulations offer sustained and targeted drug delivery to the eye, potentially improving treatment of glaucoma, dry eye, and infections. Cancer therapy: Niosomes can deliver anticancer drugs directly to tumor cells, reducing systemic side effects. Research is ongoing, with some formulations reaching clinical trials. Cosmetics: Niosomes are incorporated into various cosmetic products like sunscreens, moisturizers, and anti- aging creams due to their ability to encapsulate and deliver various ingredients effectively.
- 30. FUTURE ASPECTS OF NIOSOMES Targeted Drug Delivery: Niosomes can be further modified with specific ligands or antibodies to target specific cells or tissues, improving efficacy and reducing side effects. Combination Therapy: Combining niosomes with other drug delivery systems or therapeutic agents could offer synergistic effects for complex diseases. Controlled Release: Modifying niosomal composition can achieve controlled and sustained release of drugs, improving patient compliance and therapeutic outcomes. Gene Therapy: Niosomes are being explored as potential carriers for genetic material, offering a novel approach for gene therapy. Personalized Medicine: Tailoring niosomal formulations to individual patients based on their genetic makeup and disease characteristics holds great promise for personalized medicine.
- 31. REFERENCES 1) Okore, V.C., Attama, A.A., Ofokansi, K.C., Esimone, C.O. and Onuigbo, E.B., 2011. Formulation and evaluation of niosomes. Indian journal of pharmaceutical sciences, 73(3), p.323. 2) Srinivas, S., Kumar, Y.A., Hemanth, A. and Anitha, M., 2010. Preparation and evaluation of niosomes containing aceclofenac. Dig J Nanomater Bios, 5(1), pp.249-254.
