Brachial plexus anatomy, diagnosis and orthopaedic treatment
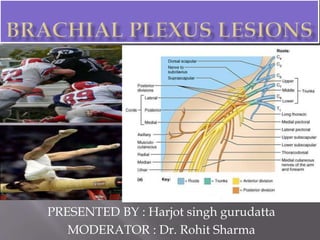
- 1. PRESENTED BY : Harjot singh gurudatta MODERATOR : Dr. Rohit Sharma
- 2. 12-2 Formed by ventral rami of spinal nerves C5-T1 Pre and post fixed Five ventral rami form three trunks that separate into six divisions that then form cords that give rise to nerves Major nerves Axillary Radial Musculocutaneous Ulnar Median
- 4. 1) Root value of lateral cord & all its branches is C5,6,7 with NO EXCEPTION. 2) Root value of medial cord & all its branches is C8 & T1 with ONE EXCEPTION; Ulnar nerve; whose root value is C7,8 & T1. 3) Root value of posterior cord branches is C5,6 with TWO EXCEPTIONS : @ Thoracodorsal nerve; C6,7,8. @ Radial nerve; C5,6,7,8 & T1. 4) Root value of upper trunk & its branches is C5,6. *Things to Notice*
- 5. Some mnemonics for remembering the branches: Posterior Cord Branches STAR - Subscapular (upper and lower), Thoracodorsal, Axillary, Radial ULTRA or ULNAR- Upper subscapular, Lower subscapular, Thoracodorsal, Radial, Axillary Lateral Cord Branches LML or LLM "Lucy Loves Me" - Lateral pectoral, Lateral root of the median nerve, Musculocutaneous Medial Cord Branches M4U or MMMUM "Most Medical Men Use Morphine" - Medial pectoral, Medial cutaneous nerve of arm, Medial cutaneous nerve of forearm, Ulnar, Medial root of the median nerve
- 6. M shape formed by 1. Musculocutaneous N. 2. Lat. & Med. Root of median N. of both lat. & med. Cords. 3. Ulnar N. 1 2 3
- 8. DERMATOMES OF UPPER LIMB
- 9. ERB’S PARALYSIS • Erb’s point • Causes Downward traction • Nerve roots involved • Muscles Paralysed • Deformity • Disability •deltoid –supraspinatus– infraspinatus–biceps -brachialis
- 11. Klumpke’s paralysis- Site of injury Cause of injury Nerve roots involved Muscles paralysed Deformity Disability
- 12. CLAW HAND HORNER SYNDROME
- 13. High-energy trauma to the upper extremity and neck causes a variety of lesions to the brachial plexus. The common mechanism is violent distraction of the entire forequarter from the rest of the body ie motorcycle accident or a high-speed motor vehicle accident. A fall from a significant height may also result in brachial plexus injury. DIRECT BLOW AND TRACTION. Sports most commonly associated with brachial plexus injuries include: Am football, baseball, basketball, volleyball, fencing, wrestling, and gymnastics Nerve injuries can result from blunt force trauma, poor posture, or chronic repetitive stress Patients generally present with pain and/or muscle weakness Over time, some patients may experience muscle atrophy Loss of useful function of the upper extremity is common
- 14. Millesi classification* Supraganglionic Infraganglionic Trunk Cord Anatomical Classification C5-6 waiters tip (Erbs palsy) C5-7 as above, elbow slightly flexed C5-T1 flail limb, claw hand, vasomotor changes, +/- Horners syndrome
- 16. Nerve root avulsion dorsal & ventral rootlets invested by pia mater / dural funnel etiology: traction (occasionally missile, knife) Significant traction causes dural rupture / root vulnerability ventral > dorsal root (esp C8-T1) at higher risk POOR Prognosis!
- 17. Grade 1 – Neuropraxia Disruption in nerve function that produces numbness and tingling Most common grade within athletics Symptoms usually resolve within several minutes Grade 2 – Axonotmesis Damage to the nerve’s axon Symptoms = numbness, tingling, and affected function (may last several days) Long nerves have a greater healing time than short nerves Rare within athletics Motor march, Tinel sign Grade 3 – Neurotmesis Permanent nerve damage occurs Very rare within athletics “Occurs with high-energy trauma, fractures, and penetrating injuries”
- 18. How do you Rx the patient knocked off his motorcycle with clavicle # and flail arm? Manage acute injury according to ATLS principles; look for concomitant injury ie c- spine. History Age, handedness, occupation, special skills Cause of injury: arm hyperabducted vs neck laterally flexed Immediate or delayed arm weakness Concomitant injury General health: PMH, DH, Smoker
- 19. Examination (use pre-printed brachial plexus diagrams): determine level Look at face: does he have Horner’s? (=lower root lesion C8 T1) Undress upper torso Look from front at posture of arm, scars, muscle wasting, asymmetry/swelling Look at back again for scars, muscle wasting, asymmetry Test sp. Accessory n (shrug shoulders) Supraspinatus responsible for 1st 20 of shoulder abduction (resisted arm abduction) Rhomboids (touch back of head) Lat dorsi (press both hands into hips and cough) Look at vascularity of arm Check sensation both upper limbs (root levels) Check movement both upper limbs from shoulder to fingers (AROM + PROM) Reflexes Function of phrenic nerve
- 22. Wall test for serratus ant (winging scapula) Note weak trapezius (asymmetric shrug)
- 23. Brachial Plexus Cervical Compression Test Cervical Distraction Test Spurling’s Test Brachial Plexus Traction Test Thoracic Outlet Syndrome Adson’s Test Allen’s Test
- 24. Axillary N. Sensory – Lateral arm Motor – Shoulder abduction Musculocutaneous N. Sensory – Anterior arm Motor – Elbow flexion Radial N. Sensory – 1st Dorsal web space Motor – Wrist extension and thumb extension Median N. Sensory – Pad of Index finger Motor – Thumb pinch and abduction Ulnar N. Sensory – Pad of little finger Motor – Finger abduction
- 25. C5 – Biceps brachii reflex (anterior arm near antecubital fossa) C6 – Supinator reflex (lateral aspect of forearm) C7 – Triceps brachii reflex (at insertion of tricep brachii) C8 and T1 do not have reflex tests
- 26. Imaging: Xray: AP chest (look for teeth and fractures ), AP + lat views shoulder, C-Spine (AP, lat, odontoid peg), Fine-cut CT, MRI
- 27. Sensory nerve action potentials (SNAPs): differentiate preganglionic from postganglionic injuries. …histamine.. Electromyography (EMG): In the first week after injury, EMG cannot be used to exclude a complete disruption unless voluntary motor unit action potentials are observed. If no signs of denervation are present in a paralyzed muscle by 3 weeks after injury, EMG can be used to confirm a neuropraxia. Somatosensory evoked potentials (SSEPs): In general, SNAPs are more reliable than SSEPs. Many difficulties exist with SSEPs, and they are not widely used.
- 28. Medical: MDT physio: maintain supple joints with FROM Orthoptists / splinting Pain control Surgical options: nerve transfers nerve grafting muscle transfers free muscle transfers neurolysis of scar in incomplete lesions Arthrodesis to stabilise joints
- 29. Open wounds Sharp injury Bullet injury Closed injuries
- 30. Chest tube
- 32. Bullet woundClavicle osteotomy Junction of trunk and cords
- 33. Laceration
- 34. Nerve repair and graft
- 35. Laceration
- 36. Nerve graft
- 37. Closed injury, (tractional injuries)
- 38. Closed injury, (tractional injuries) Early exploration Underobservation Decision for the time of delay exploration Decision for the type of the treatment Late recostruction
- 39. Closed injury, (tractional injuries) Early exploration Underobservation Decision for the time of delay exploration Decision for the type of the treatment Late recostruction Peripheral reconstruction
- 40. Closed injury, (tractional injuries) Early exploration vascular reconstruction
- 41. Closed injury, (tractional injuries) Early exploration Underobservation First 6-12 weeks Stabilization of the patient Stabilization of the injury Evaluation of the improvement After 2-3 months No improvement; exploration Progressive improve; wait & watch Non-anatomic recovery; explor. Based on severity
- 42. Closed injury, (tractional injuries) Early exploration Underobservation Decision for the time of delay exploration No recovery After 6-12 weeks (based on the severity of the trauma) Progressive improvement Wait for further improvement Non-anatomic recovery Exploration before 9-12 months
- 43. Closed injury, (tractional injuries) Early exploration Underobservation Decision for the time of delay exploration Decision for the type of the treatment
- 44. Neurolysis Nerve repair Nerve graft Nerve transfer Tendon transfer Arthrodesis Functional muscle flaps Straight on Brachial Plexus Early exploration Delay exploration Peripheral reconstruction Late reconstruction Danger of more damage Failure is obvious
- 45. Neurolysis….check…potential Nerve repair Nerve graft Nerve transfer Tendon transfer Arthrodesis Functional muscle flaps
- 46. Gun shot injury
- 47. After neurolysis from scar tissue
- 48. Neurolysis Nerve repair… Nerve graft Nerve transfer Tendon transfer Arthrodesis Functional muscle flaps
- 49. Neurolysis Nerve repair Nerve graft Nerve transfer Tendon transfer Arthrodesis Functional muscle flaps Sural medial cutaneous forearm ulnar (vascularised) Self transfer (i.e. Sural Nerve) Manufactured Nerve Processed Nerve Cadaver Transplant Living Related Transplant
- 52. Neurolysis Nerve repair Nerve graft Nerve transfer..neurotization Tendon transfer Arthrodesis Functional muscle flaps Accessory nerve Cervical plexus Phrenic nerve Intercostal nerves Ulnar ECU nerve Crossed C7 Hypoglossal nerve
- 53. Motor cycle accident open wound
- 55. Accessory to suprascapular
- 57. Oberlin nerve transfer
- 58. Oberlin nerve transfer Biceps m. Ulnar n. Anastamosis
- 59. Radial to axillary transfer
- 61. ICN 4 ICN 5 ICN 6 Musclocutaneus n
- 62. Neurolysis Nerve repair Nerve graft Nerve transfer Tendon transfer Arthrodesis Functional muscle flaps
- 64. Triceps to Biceps
- 68. Latismus dorsi transfer to flexion elbow and extension finger
- 71. Trapez to Deltoid
- 72. Neurolysis Nerve repair Nerve graft Nerve transfer Tendon transfer Arthrodesis Functional muscle flaps
- 74. Shoulder arthrodesis in BPI
- 75. Neurolysis Nerve repair Nerve graft Nerve transfer Tendon transfer Arthrodesis Functional muscle flaps
- 76. Gracillis harvest Accessory n.
- 77. First stage of Doi procedure
- 78. Partial ulnar n. as a donor nerve
- 80. Extra plexus donor
- 81. Brachial plexus injury Open sharp injury Shot gun Tractional injury Immediate exploration under observation Exploration No improvement in 2-3 m Explor. In 12 m. Non-anatomic improvement Peripheral reanimation > 12m . Gradual improvement
- 83. Root value- C5 Supply – Rhomboid major & minor muscle Posterior view
- 84. LONG THORACIC NERVE Root value- C5,C6,C7 Supply – Serratus anterior muscle
- 85. BRANCHES OF UPPER TRUNK NERVE TO SUBCLAVIUS Root value – C5,C6 SUPRASCAPULAR NERVE Root value – C5,C6
- 86. Root value- C5,C6,C7 MEDIAL PECTORAL NERVE Root value- C8,T1
- 87. MUSCULOCUTANEOUS NERVE Root value – C5,C6,C7
- 89. MEDIAL CUTANEOUS NERVE OF ARM Root value- C8,T1 MEDIAL CUTANEOUS NERVE OF FOREARM Root value- C8,T1
- 91. UPPER SUBSCAPULAR Root value-C5,C6 LOWER SUBSCAPULAR Root value- C5,C6 NERVE TO LATISSIMUS DORSI Root value-C6,C7,C8
- 92. AXILLARY NERVE
- 93. RADIAL NERVE
- 97. Test for ulnar nerve Card test Froment’s sign Egawa’s test
- 98. CONTENT Axillary artery & its branches Axillary vein & its tributaries Infraclavicular part of brachial plexus Axillary lymph nodes Axillary fat
- 99. Carpal tunnel syndrome Epidemiology Signs &symptoms Motor changes Sensory changes Vasomotor changes Trophic changes
- 100. Tests done Tinel sign Phalen’s maneavure
- 101. Radial Nerve Injury in axilla • Causes of injury Motor effects:paralysis of triceps,anconeus extensors of the wrist Extensors of fingers. Brachioradialis supinator muscle • Deformity: Wrist and finger drop Sensory effects -small area of sensation loss at arm andforearm sensory loss over lateral part of the dorsum of the hand (lat. 3.5 fingers without distal phalynges)
- 102. Injuries at Spiral Groove Caused by fracture shaft of humerus. • Motor effects: paralysis of extensors of the wrist Extensors of fingers • Deformity: Wrist and finger drop • Sensory effects: anesthesia is present over the dorsal surface of the hand (lat. 3.5 fingers)
- 105. 12-105 Spinal nerves attach to the spinal cord via roots Dorsal root Has only sensory neurons Attached to cord via rootlets Dorsal root ganglion Bulge formed by cell bodies of unipolar sensory neurons Ventral root Has only motor neurons No ganglion - all cell bodies of motor neurons found in gray matter of spinal cord
- 106. 12-106 31 pair each contains thousands of nerve fibers All are mixed nerves have both sensory and motor neurons) Connect to the spinal cord Named for point of issue from the spinal cord 8 pairs of cervical nerves (C1-C8) 12 pairs of thoracic nerves (T1-T12) 5 pairs of lumbar nerves (L1-L5) 5 pairs of sacral nerves (S1-S5) 1 pair of coccygeal nerves (Co1)
- 107. 12-107 Rami are lateral branches of a spinal nerve Rami contain both sensory and motor neurons Two major groups Dorsal ramus Neurons innervate the dorsal regions of the body Ventral ramus Larger Neurons innervate the ventral regions of the body Braid together to form plexuses (plexi)
- 108. 12-108 Spinal nerves indicated by capital letter and number Dermatomal map: skin area supplied with sensory innervation by spinal nerves
- 109. 12-109 Nerve plexus A network of ventral rami Ventral rami (except T2-T12) Branch and join with one another Form nerve plexuses In cervical, brachial, lumbar, and sacral regions No plexus formed in thoracic region of s.c.
- 110. 12-110 Dorsal Ramus Neurons within muscles of trunk and back Ventral Ramus (VR) Braid together to form plexuses Cervical plexus - VR of C1-C4 Brachial plexus - VR of C5-T1 Lumbar plexus - VR of of L1-L4 Sacral plexus - VR of L4-S4 Coccygeal plexus -VR of S4 and S5 Communicating Rami: communicate with sympathetic chain of ganglia Covered in ANS unit
- 111. 12-111 Formed by ventral rami of spinal nerves C5-T1 Five ventral rami form three trunks that separate into six divisions that then form cords that give rise to nerves Major nerves Axillary Radial Musculocutaneous Ulnar Median
